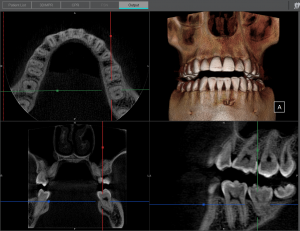
A shielding study is often one of the most confusing parts of setting up a cone beam system. Many dental offices do not understand the process, and equipment service technicians are often the first people they turn to for help.
A shielding study is often one of the most confusing parts of setting up a cone beam system. Many dental offices do not understand the process, and equipment service technicians are often the first people they turn to for help.
When you can explain the shielding review process in plain language, what’s required, what’s optional, what drives recommendations, and what information really matters, you become more than “the repair person.” You become the person who helps the office avoid delays, cost surprises, and compliance headaches. Below are several commonly misunderstood facts that can help you guide your dental customers more confidently.
Some states require shielding studies, and some don’t
Shielding requirements are not uniform across the U.S. Some states require a shielding evaluation for dental CBCTs. Some even require it for other modalities, like pan ceph systems as well. Even when a state doesn’t require a shielding study, there can still be value in doing one. As a technician, simply knowing whether a state is strict, moderate, or hands-off can help set expectations early, especially when timelines are tight.
Most states have approved physicists, and some vendors cover many states
In states that regulate shielding reviews, there’s often a list for qualified or approved radiation physicists to perform the evaluation. In addition, there are larger companies that operate across multiple states and handle shielding reviews as a routine service. For instance, Landauer is a larger company that can perform shield reviews nationally.
Shielding reviews focus heavily on employee safety, not just patient exposure
Most radiation physicists will request some kind of drawing not only of the room where the unit will be located, but also the surrounding area. One of the items they are reviewing is whether there may be “stationary” employees located near the machine. This can be counterintuitive to dental teams. Patients are absolutely important, but staff may be in or near the area all day, every day. For instance, a classic red-flag scenario is a dental cone beam in close proximity (e.g. on the other side of the wall) to the front desk. The concern is that staff members may be located close to the unit all day, and they may not even know scans are happening.
The trigger switch location matters more than people expect
A shielding review often asks to identify on the drawing where the exposure switch or trigger will be located. The reason they look at this is to estimate where the operator stands during exposures, and therefore the likely long-term exposure profile for the person who runs the scans.
State rules exist, but the physicist’s judgment plays a big role
Even in regulated states, there can be gray area. Many shielding decisions involve professional judgment based on distance to occupied areas, expected workload, type of unit and scan protocols, and construction details like wall composition. The good news is that most radiation physicists are practical. They know dentists aren’t trying to build a hospital bunker, and they usually aim for recommendations that are feasible and cost-effective if they have good information to work with.
What’s above and below the room can play a role
A common question with shielding reviews is what’s above and below the imaging room. That’s because shielding isn’t only about what’s on the other side of the wall. Vertical adjacency matters too.
Examples that can change calculations include office space above or below with staff present all day, residential space above or below in a mixed-use building, or storage and mechanical spaces that typically have lower occupancy. If your customer is in a multi-tenant building, this topic alone can prevent major surprises.
Many shielding studies are done remotely, without a site visit
Another misconception is that the physicist must come onsite. Many evaluations can be completed remotely using room drawings or floor plans, dimensions and wall compositions, proposed equipment placement and orientation, and adjacency and occupancy information. Site visits do happen, especially for complex spaces, unclear construction, or post-install verification, but remote reviews are common and can be faster.
Shielding isn’t “lead or nothing.” Distance and materials matter
Lead is very good shielding material, but it’s not the only barrier that is available. Physicists typically account for existing drywall layers, distance and geometry to help ensure compliance.
For instance, distance can be a great protection because radiation intensity drops rapidly as you move away from the source. A simplified rule of thumb many people relate to is the inverse-square relationship, where doubling distance can reduce exposure to roughly one-quarter, depending on scatter conditions and layout. So yes, an operator 8 feet away receives dramatically less exposure than someone 1 foot away, even before you factor in walls or shielding.
The practical takeaway is that a good shielding review doesn’t always mean “add lead everywhere.” Sometimes the best fix is layout, operator position, or recognizing that existing construction already provides meaningful attenuation.
The physicist needs specific machine data, especially operating parameters and scatter information
For CBCT and other dental imaging systems, the shielding review typically requires details about the unit such as maximum kVp, maximum mA, and sometimes exposure time or duty cycle assumptions, plus workload estimates like scans per week or day, or orientation.
Many physicists also ask for manufacturer documentation describing scatter or radiation distribution around the unit. People often call this a scatter plot, although terminology can vary by manufacturer and physicist. The point is the same: the physicist needs a credible basis for how radiation propagates in the room so they can model exposure.
Moving equipment may trigger a new study, even within the same building
Some states require a new shielding evaluation when equipment is moved to a different room, the orientation changes significantly, adjacent occupancy changes, or sometimes even when the unit is relocated within the same facility. Offices are often surprised by this because it’s the same machine, but from a safety standpoint, the exposure environment can change completely based on layout and occupancy.
Conclusion
Shielding reviews don’t have to be mysterious, and they’re rarely just “how much lead is in the wall.” They’re a practical risk assessment shaped by occupancy, distance, adjacent spaces, operator position, and machine parameters, all things you already think about when planning installs and service work.
When you can explain these realities to a dentist or office manager and help them gather the right info for the physicist, you’re saving them time, preventing delays, and reducing the chance of expensive last-minute construction changes.
About ImageWorks
ImageWorks provides imaging systems that deliver excellent image quality, competitive pricing, and dependable performance without the headaches. We help dental professionals and technicians install and use imaging equipment with confidence and simplicity.


 A shielding study is often one of the most confusing parts of setting up a cone beam system. Many dental offices do not understand the process, and equipment service technicians are often the first people they turn to for help.
A shielding study is often one of the most confusing parts of setting up a cone beam system. Many dental offices do not understand the process, and equipment service technicians are often the first people they turn to for help. 
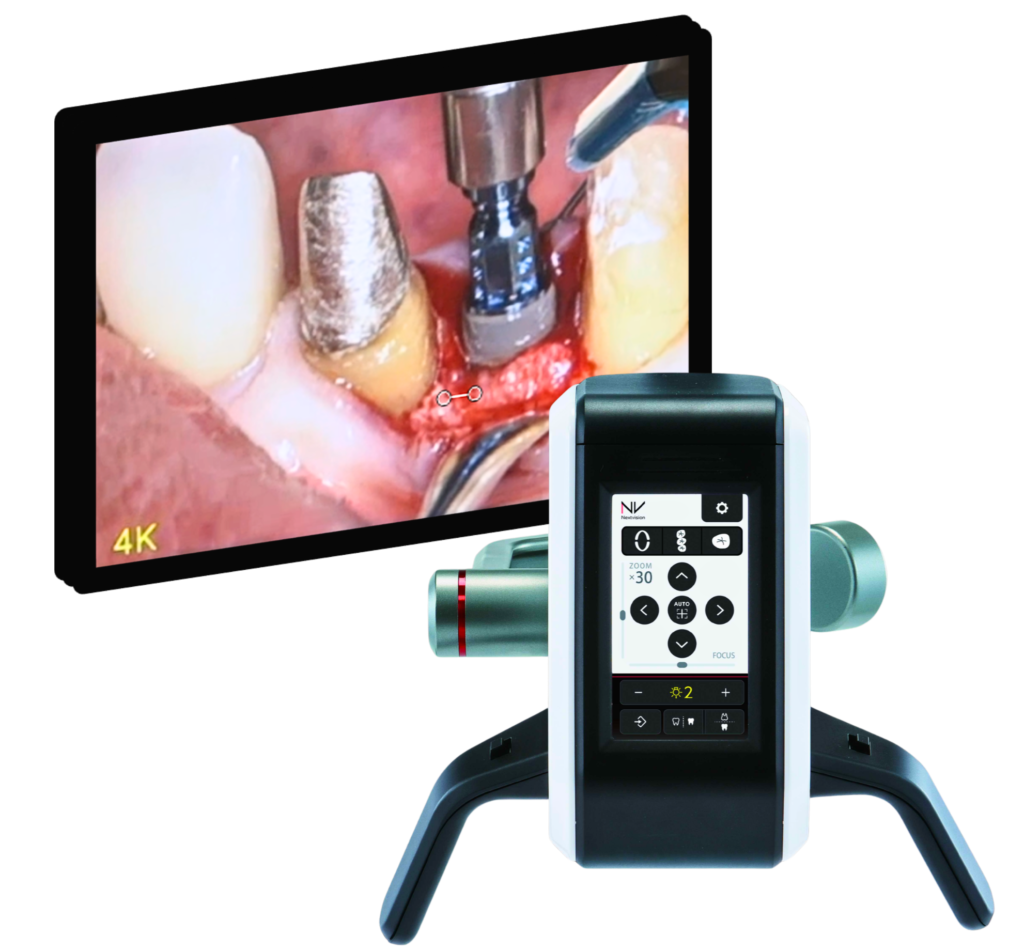 The Mielscope can make your dental practice more productive, persuasive, and profitable without adding complexity. This innovative dental microscope system replaces outdated tools, captures powerful imagery, and enhances communication. It offers high-magnification visibility without causing neck strain or interrupting your clinical workflow.
The Mielscope can make your dental practice more productive, persuasive, and profitable without adding complexity. This innovative dental microscope system replaces outdated tools, captures powerful imagery, and enhances communication. It offers high-magnification visibility without causing neck strain or interrupting your clinical workflow.